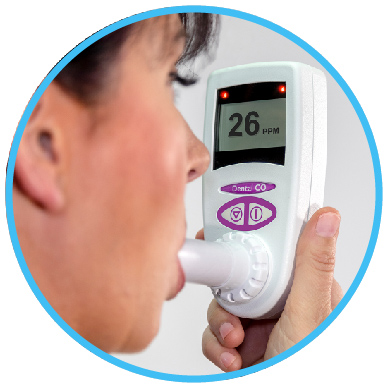
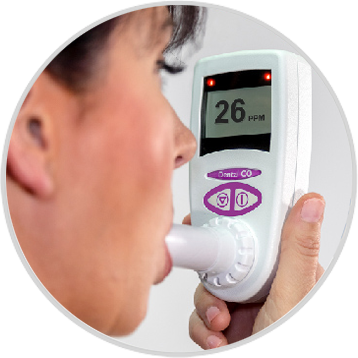
USER ADVANTAGES:
- Results instantly displayed
- Single press button to toggle between ppm and %COHb
- Breath hold countdown timer to guide patients
- Coloured light indicators to signify smoking level
- Supplied with Safebreath mouthpieces to ensure a complete hygiene concept
References:
1. Anczakj, Nogler (2003). Tobacco cessation in primary care: maximizing intervention strategies. Clinical Medicine & Research 2003; 1: 201–216.
2. Fu S, Partin M, Snyder A, An LC, Nelson DB, Clothier B, Nugent S, Willenbring ML, Joseph AM. (2006) Promoting repeat tobacco dependence treatment: are relapsed smokers interested? American Journal of managed Care 2006; 12 235–243.
3. Smoking Toolkit Study (2001) Available at: http://www.smokinginengland.info/
4. Slama KJ, Redman S, Cockburn J, Sanson-Fisher R. Community views about the role of general practitioners in disease prevention. Family Practice 1989; 6: 203–209.
5. Department of Health (2009), Stop Smoking Interventions in Secondary Care. Available online: www.ncsct.co.uk/Content/FileManager/documents/NCSCT-CIC-Delivery-Projects/ Secondary-care/stop-smoking-interventions-in-secondary-care-guidance-oct09.pdf
6. Carr AB, Ebbert J. Interventions for tobacco cessation in the dental settings. Cochrane Database of Systematic Reviews 2012, Issue 6. Art. No.: CD005084. DOI: 10.1002/14651858.CD005084.pub
7. Warnakulasuriya S, Dietrich T, Bornstein MM, Casals PE, Preshaw PM, Walter C et al. Oral health risks of tobacco use and effects of cessation. International Dental Journal 2010; 60(1):7–30.
8. The health consequences of smoking – 50 Year of Progress. A Report of the Surgeon General. Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health, 2014. https://www.surgeongeneral.gov/library/reports/50-years-of-progress/full-report.pdf
References:
9. Morse DEK. Smoking and drinking in relation to oral epithelial dysplasia. Cancer Epidemiology Biomarkers and Prevention 1996; 5(10):769–777.
10. Kulasegaram R, Downer MC, Jullien JA, et al. Care-control study of oral dysplasia and risk habits among patients of a dental hospital. Eur J Cancer B Oral Oncol 1995; 31B(4):227–231.
11. Bergstrom J. Periodontitis and smoking: an evidence-based appraisal. Review. J Evid Based Dent Pract 2006;6:33–41.
12. Johnson GK, Guthmiller JM. The impact of cigarette smoking on periodontal disease and treatment. Periodontol 2000 2007;44:178–94.
13. Chatzopoulos G. Smoking, Smokeless Tobacco, and Alcohol Consumption as Contributing Factors to Periodontal Disease. Northwest Dent. 2016 Jan–Feb;95(1):37–41.
14. Tomar SL, Asma S, Tomar SL, Asma S. Smoking-attributable periodontitis in the United States: findings from NHANES III. National Health and Nutrition Examination Survey. Journal of Periodontology 2000; 71(5):743–751.
15. Ismail AI, Burt BA, EKlund SA. Epidemiological patterns of smoking and periodontal disease in the United States. J Am Dent Assoc 1983; 106:617–612.
16. Bergstrom JE. A 10-year prospective study of tobacco smoking and periodontal health. Journal of Periodontology 2000; 71(8):1338–1347.
17. Doll R, Peto R, Boreham J, Sutherland I. Mortality in relation to smoking: 50 years’ observations on male British doctors. BMJ 2004; 328:1519.
18. Preshaw PM, Heasman L, Stacey F, Steen N, McCracken GI, Heasman PA et al. The effect of quitting smoking on chronic periodontitis. Journal of Clinical Periodontology 2005; 32(8):869–879.
19. Hilgers KK, Kinane DF, Hilgers KK, Kinane DF. Smoking, periodontal disease and the role of the dental profession. International journal of dental hygiene 2004; 2(2):56–63.
20. Delima SL, McBride RK, Preshaw PM, Heasman PA, Kumar PS, Delima SL et al. Response of subgingival bacteria to smoking cessation. Journal of Clinical Microbiology 2010; 48(7):2344–2349.
![]()